 Diabetic foot ulcers can be incredibly dangerous, leading to life-threatening amputations and other long-term health issues if left untreated. This article will examine the causes, risk factors, diagnosis procedure, treatments and preventive care for these ulcers. It is crucial for diabetics to understand the potentially devastating implications of an unchecked ulcer in the foot so that it can be efficiently diagnosed and adequately treated in time.
Diabetic foot ulcers can be incredibly dangerous, leading to life-threatening amputations and other long-term health issues if left untreated. This article will examine the causes, risk factors, diagnosis procedure, treatments and preventive care for these ulcers. It is crucial for diabetics to understand the potentially devastating implications of an unchecked ulcer in the foot so that it can be efficiently diagnosed and adequately treated in time.
Understanding Diabetic Foot Ulcers
By recognizing the symptoms and improving living conditions it is possible to lessen the severity of future diabetic foot ulcers or even prevent them from occurring in the first place. While prevention is undoubtedly preferable than dealing with severe consequences caused by a ulcer in the foot once it has formed, understanding diagnosis, treatment options, and potential complications will empower readers to take charge of their own health and well-being.

What Causes Diabetic Ulcerations on the Feet?
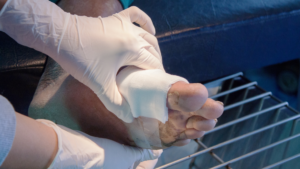 It is not tough to understand why people with diabetes often experience ulceration in their feet. Not only do they have to deal with diminished circulation in their extremities, the lack of feeling caused by nerve damage means there is reduced ability to detect trauma incurred from simple daily activities such as walking or even just having shoes on too tight. Above all, this leads to increased pressure being placed in one certain area leading to tissue damage and open sores that can be extremely difficult for sufferers of diabetes to manage and contain without proper medical care. Diabetic foot ulceration can cause major health issues if it is not addressed efficiently, which is why its prevention should be taken very seriously.
It is not tough to understand why people with diabetes often experience ulceration in their feet. Not only do they have to deal with diminished circulation in their extremities, the lack of feeling caused by nerve damage means there is reduced ability to detect trauma incurred from simple daily activities such as walking or even just having shoes on too tight. Above all, this leads to increased pressure being placed in one certain area leading to tissue damage and open sores that can be extremely difficult for sufferers of diabetes to manage and contain without proper medical care. Diabetic foot ulceration can cause major health issues if it is not addressed efficiently, which is why its prevention should be taken very seriously.
Risk factors for an Ulcer in the Foot
Foot ulcers due to diabetes can be a serious and ongoing problem for individuals affected. These ulcerations are caused by a variety of factors; for example, neuropathy and bunions, limited blood flow or ischemia, obesity, history of previous foot ulcers, high glucose levels in the bloodstream and smoking habits. Many people with diabetes know to watch out for these factors as they can contribute to an increased risk of developing a diabetic foot ulcer.
Additionally, tight fitting shoes don’t allow for proper circulation and may further increase the chances of developing this condition and should therefore be avoided. By being aware of all the possible sources triggering diabetic foot ulcers and closely monitoring potential risk factors, many affected individuals can reduce their chance of developing these painful wounds.
Diagnosis of Diabetic Foot Ulcers
Early diagnosis and detection of diabetic foot ulcers is a critical step in providing effective treatment. Besides taking a thorough physical examination of the feet and listeners for any symptoms, expert podiatrists may order multiple tests to accurately assess the condition.
From vascular studies that gauge blockages or disrupts in blood flow to neurological examinations checking for any reduction in sensation in the toes, numerous medical exams can be done. Additionally, advanced imaging tests such as CT scans or X-rays can detect tissue damage and other potential health risks associated with the ulcer. By working with their foot doctors, patients are then able to begin taking control of their health to get back on track.

Diabetic Foot Ulcer Stages – Early Stage vs. Late Stage
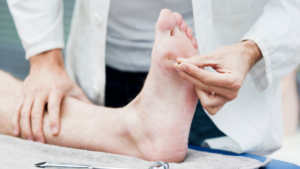 When dealing with diabetic foot ulcers, it’s crucial to have an understanding of the natural progression of diabetic foot disease, which can be classified into five stages. These stages include: a normal foot, a high-risk foot, an ulcerated foot, an infected foot, and a necrotic foot. The development of a foot ulcer is a significant event in stage 3 and requires urgent and aggressive treatment.
When dealing with diabetic foot ulcers, it’s crucial to have an understanding of the natural progression of diabetic foot disease, which can be classified into five stages. These stages include: a normal foot, a high-risk foot, an ulcerated foot, an infected foot, and a necrotic foot. The development of a foot ulcer is a significant event in stage 3 and requires urgent and aggressive treatment.
Proper management of diabetic foot care across all stages requires a multidisciplinary approach to address mechanical, wound, microbiological, vascular, metabolic, and educational aspects. Maintaining good control of blood glucose, lipids, and blood pressure is essential in every stage, as is educating patients on proper foot care appropriate for each stage.
Early Stage Diabetic Foot Ulcer
Ideally, preventing the development of ulcers should be the primary focus during stages 1 and 2. In stage 1, encouraging the use of suitable footwear and educating patients on healthy foot care and footwear habits is critical. In stage 2, patients have developed one or more risk factors for ulceration, including neuropathy, ischaemia, deformity, swelling, and callus. Most deformities can be accommodated in special footwear, and callus should be treated aggressively, particularly in the neuropathic foot.
Middle Stage Ulcer on the Foot
During stage 3, ulcers can be classified into two categories: those in the neuropathic foot and those in the neuroischaemic foot. In the neuropathic foot, ulcers commonly occur on the plantar surface of the foot and toes and are associated with neglected callus and high plantar pressures. In the neuroischaemic foot, ulcers are typically seen around the edges of the foot and are associated with trauma or wearing unsuitable shoes. Relief of pressure, sharp debridement and dressings, and possibly vascular intervention for neuroischaemic foot ulcers are necessary for proper treatment.
Final Stage Ulcer
In stage 4, microbiological control is crucial, and severe infections require intravenous antibacterial therapy and prompt assessment for surgical drainage and debridement. If left untreated, severe infections may progress to necrosis in stage 5, which can be classified as wet or dry necrosis. Aggressive management, including intravenous antibacterials and surgical debridement, is necessary for treating wet necrosis in neuropathic feet, and vascular reconstruction is often required for neuroischaemic feet. Effective management of diabetic foot ulcers can help reduce the number of feet that progress to infection and necrosis, ultimately decreasing the number of major amputations in diabetic patients.
A Wound Care Specialist Near You Can Help!
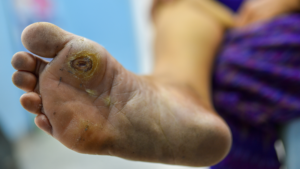 In the case of diabetic foot ulcers, tailoring treatment can be particularly important. Each patient is unique and experiences different levels of intensity, placement and discomfort. Custom orthotics or specialized footwear are two proven methods to reduce pressure on affected areas, defined by a Podiatrist’s expertise and knowledge of the patient’s needs. The ultimate goal is to facilitate healing without creating more issues or inviting infection, carefully monitored during any relevant treatment plan. In addition, avoidance strategies such as regular foot checks are recommended with diabetic patients in order to detect signs of trouble early on before they spiral out of control.
In the case of diabetic foot ulcers, tailoring treatment can be particularly important. Each patient is unique and experiences different levels of intensity, placement and discomfort. Custom orthotics or specialized footwear are two proven methods to reduce pressure on affected areas, defined by a Podiatrist’s expertise and knowledge of the patient’s needs. The ultimate goal is to facilitate healing without creating more issues or inviting infection, carefully monitored during any relevant treatment plan. In addition, avoidance strategies such as regular foot checks are recommended with diabetic patients in order to detect signs of trouble early on before they spiral out of control.
Preventing Ulcers
It is paramount that those with diabetes maintain a rigorous routine of foot inspections. Early detection and treatment are instrumental towards ensuring the proper healing of a wound. This process should become like second nature and consist of closely inspecting your feet daily for cuts, abrasions or any kind of discoloration of the skin so as to catch it early before it turns into something more serious. With small preventive measures such as these, we can all work together in helping individuals deal with the struggles associated with diabetes- seek medical assistance when necessary and look out for one another!
Eating healthily and exercising regularly are important for keeping your blood sugar at a healthy level, thereby preventing diabetic foot ulcers from occurring. However, simply eating healthily and exercising won’t guarantee the prevention of these ulcers if proper-fitting shoes are not worn. This is because excess pressure on particular parts of the feet can lead to wounds over time, potentially with significantly severe consequences if they are left untreated. Making sure to wear comfortable shoes that fit correctly is an easy way to prevent these types of sores from forming in the first place.
It is essential to take several steps in order to ensure optimal protection for your feet. Keeping them both clean and dry is pivotal, as dirt or sweat can lead to adverse skin conditions. Going without shoes in public places carries with it the risk of injury and should be avoided. Regularly trimming one’s nails serves as an effective defense against ingrown nails, which can prove to be quite painful over time. Applying lotion routinely is also noteworthy, maintaining the skin’s moisture level while averting any possible side effects such as cracking or peeling. Rest assured that by taking the above mentioned precautions, you will be able to lessen potential harm and keep your feet feeling healthy and strong!





